Shingles vaccine may reduce dementia risk by 20% as new study makes ‘striking finding’
The new research is a huge step towards preventive treatment for dementia.
A new study has made the “striking finding” that a certain vaccine can reduce the risk of dementia by a staggering 20 per cent. The research project led by Stanford Medicine involved analysing the health records of Welsh older adults.
It was discovered that those who received the shingles vaccine were a fifth less likely to develop dementia over the next seven years when compared to those who did not receive the vaccine.
These results, published in scientific journal Nature, have strengthened a previously-found link between viruses that affect the nervous system and the increase of dementia risk. It is thought that the study is a step towards new preventive intervention for dementia.
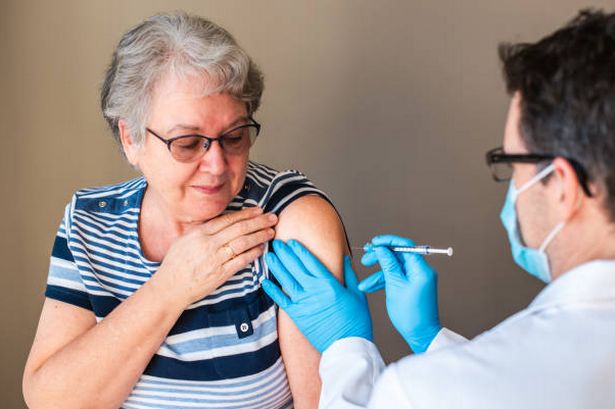
Shingles is a viral infection that produces a painful rash and is caused by the same virus as chickenpox. In people who have had chickenpox, usually in childhood, the virus stays dormant in their nerve cells for life.
For older people, or those with weakened immune systems, the dormant virus can reactivate and cause shingles.
Dementia affects more than 55 million people worldwide, with an estimated 10million new cases every year. In Scotland, an estimated 90,000 people live with dementia, according to the Scottish Government.
In this new study, the researchers looked at the health records of more than 280,000 adults aged 71 to 88 years old who did not have dementia at the start of the vaccination program, which began in 2013.
The shingles vaccine eligibility threshold was 80, so the team focused their analysis on those closest to either side of this, e.g. selecting people who were 79 and had one year left of eligibility for the jag.
Over the next seven years, the researchers compared the health outcomes of people closest in age who were eligible and ineligible – those already aged over 80 at the beginning of the study – to receive the vaccine.
The vaccine reduced the occurrence of shingles over that seven-year period by about 37 per cent for people who received the vaccine, similar to what had been found in clinical trials.
By 2020, one in eight older adults, who were by then 86 and 87, had been diagnosed with dementia. But those who received the shingles jag were 20 per cent less likely to develop dementia than the unvaccinated.
Pascal Geldsetzer, MD, PhD, is an assistant professor of medicine and was senior author of the new study. He said: “It was a really striking finding. This huge protective signal was there, any which way you looked at the data.”
His team analysed the data in alternate ways, by using different age ranges or looking only at deaths attributed to dementia, for example, but the link between vaccination and lower dementia rates remained. “The signal in our data was so strong, so clear and so persistent,” he said.
The study also showed that protection against dementia was much more pronounced in women than in men. This could be due to sex differences in immune response or in the way dementia develops, the scientist said. Women on average have higher antibody responses to vaccination, and shingles is more common in women than in men.
Exactly how the vaccine prevents dementia- whether it increases the overall immune system, specifically reduces reactivations of the virus or prevents the condition in some other way- is still unknown.
Also unknown is whether a newer version of the vaccine, which contains only certain proteins from the virus and is more effective at preventing shingles, may have a similar or even greater impact on dementia.
Geldsetzer hopes the new findings will inspire more funding for this line of research.